When Can You Find Out the Sex of the Baby Through Blood Test
-
Genetic Screening
-
First Trimester
-
2d Trimester
-
Ultrasound
-
Amniocentesis
-
Chorionic Villus Sampling
-
Fetal Monitoring
-
Glucose
-
Group B Strep Civilization
Your health care provider may recommend a variety of screenings, tests and imaging techniques during your pregnancy. These tests are designed to provide information almost the health of your baby and may assistance you optimize your kid's prenatal intendance and evolution.
Genetic Screening
Many genetic abnormalities can exist diagnosed before nascency. Your doctor or midwife may recommend genetic testing during pregnancy if you or your partner has a family history of genetic disorders. You may besides choose to have genetic screening if you have had a fetus or babe with a genetic abnormality.
Examples of genetic disorders that can exist diagnosed before birth include:
-
Cystic fibrosis
-
Duchenne muscular dystrophy
-
Hemophilia A
-
Polycystic kidney disease
-
Sickle jail cell disease
-
Tay-Sachs illness
-
Thalassemia
The following screening methods are bachelor during pregnancy:
-
Alpha-fetoprotein (AFP) test or multiple marker examination
-
Amniocentesis
-
Chorionic villus sampling
-
Cell-gratuitous fetal Deoxyribonucleic acid testing
-
Percutaneous umbilical blood sampling (withdrawing a pocket-sized sample of the fetal blood from the umbilical cord)
-
Ultrasound browse
Beginning Trimester Prenatal Screening Tests
First trimester screening is a combination of fetal ultrasound and maternal blood testing. This screening process tin help determine the chance of the fetus having certain birth defects. Screening tests may exist used alone or with other tests.
First trimester screening includes:
-
Ultrasound for fetal nuchal translucency. Nuchal translucency screening uses an ultrasound to examine the surface area at the back of the fetal cervix for increased fluid or thickening.
-
Ultrasound for fetal nasal bone determination. The nasal os may not exist visualized in some babies with certain chromosome abnormalities, such equally Down's syndrome. This screen is performed using an ultrasound between eleven and 13 weeks gestation.
-
Maternal serum (blood) tests. These blood tests measure two substances found in the blood of all pregnant women:
-
Pregnancy-associated plasma protein A. A protein produced past the placenta in early on pregnancy. Aberrant levels are associated with an increased chance of chromosomal aberration.
-
Human chorionic gonadotropin. A hormone produced past the placenta in early on pregnancy. Abnormal levels are associated with an increased risk of chromosomal aberration.
-
When used together equally first trimester screening tests, nuchal translucency screening and maternal blood tests have a greater ability to determine if the fetus might accept a nascency defect, such every bit Downwards syndrome (trisomy 21) and trisomy 18.
If the results of these start trimester screening tests are abnormal, genetic counseling is recommended. Additional testing, such as chorionic villus sampling, amniocentesis, prison cell-free fetal DNA or other ultrasounds, may be needed for an accurate diagnosis.
Second Trimester Prenatal Screening Tests
Second trimester prenatal screening may include several blood tests called multiple markers. These markers provide information about your potential risk of having a infant with certain genetic conditions or birth defects. Screening is usually done past taking a sample of your claret between fifteen and 20 weeks of pregnancy (16 to 18 weeks is ideal). The multiple markers include:
-
AFP screening. Also called maternal serum AFP, this blood test measures the level of AFP in your blood during pregnancy. AFP is a protein normally produced by the fetal liver that is present in the fluid surrounding the fetus (amniotic fluid). It crosses the placenta and enters your blood. Abnormal levels of AFP may signal:
-
A miscalculated due appointment, as the levels vary throughout pregnancy
-
Defects in the intestinal wall of the fetus
-
Down syndrome or other chromosomal abnormalities
-
Open up neural tube defects, such as spina bifida
-
Twins (more than one fetus is producing the protein)
-
-
Estriol. This is a hormone produced by the placenta. It tin exist measured in maternal claret or urine to be used to determine fetal health.
-
Inhibin. This is a hormone produced by the placenta.
-
Human being chorionic gonadotropin. This is likewise a hormone produced past the placenta.
Abnormal examination results of AFP and other markers may mean that additional testing is needed. An ultrasound is used to confirm the milestones of your pregnancy and to check the fetal spine and other body parts for defects. An amniocentesis may exist needed for an accurate diagnosis.
Since multiple marker screening is not diagnostic, it is not 100 percent accurate. Information technology helps determine who in the population should be offered boosted testing during pregnancy. False-positive results may indicate a problem when the fetus is actually healthy. On the other hand, false-negative results indicate a normal result when the fetus really does take a health problem.
When you have both first and second trimester screening tests performed, the power of the tests to observe an abnormality is greater than using just one screening independently. Near cases of Down syndrome tin can exist detected when both first and 2nd trimester screenings are used.
Ultrasound

An ultrasound scan is a diagnostic technique that uses high-frequency audio waves to create an prototype of the internal organs. A screening ultrasound is sometimes done during the course of your pregnancy to check normal fetal growth and verify the due date.
When are ultrasounds performed during pregnancy?
Ultrasounds may be done at diverse times throughout pregnancy for several reasons:
First Trimester
-
To establish the due date (this is the near authentic manner of determining the due date)
-
To determine the number of fetuses and identify placental structures
-
To diagnose an ectopic pregnancy or miscarriage
-
To examine the uterus and other pelvic anatomy
-
To detect fetal abnormalities (in some cases)
Midtrimester (also called the 18- to 20-week scan)
-
To confirm the due date (a due date set in the first trimester is rarely changed)
-
To determine the number of fetuses and examine the placental structures
-
To assist in prenatal tests, such every bit an amniocentesis
-
To examine the fetal anatomy for abnormalities
-
To check the amount of amniotic fluid
-
To examine claret flow patterns
-
To observe fetal behavior and activity
-
To measure out the length of the cervix
-
To monitor fetal growth
Third Trimester
-
To monitor fetal growth
-
To check the amount of amniotic fluid
-
To bear the biophysical profile test
-
To decide the position of the fetus
-
To assess the placenta
How is an ultrasound scan performed?
Ii types of ultrasounds can be performed during pregnancy:
-
Intestinal ultrasound. In an abdominal ultrasound, gel is applied to your abdomen. The ultrasound transducer glides over the gel on the abdomen to create the image.
-
Transvaginal ultrasound. In a transvaginal ultrasound, a smaller ultrasound transducer is inserted into your vagina and rests against the dorsum of the vagina to create an prototype. A transvaginal ultrasound produces a sharper image than an abdominal ultrasound and is often used in early pregnancy.
Which ultrasound imaging techniques are available?
In that location are several types of ultrasound imaging techniques. As the most common type, the 2-D ultrasound provides a flat picture show of one aspect of the baby.
If more than information is needed, a iii-D ultrasound examination can be washed. This technique, which provides a 3-D movie, requires a special motorcar and special grooming. The 3-D paradigm allows the health care provider to see the width, height and depth of the images, which tin be helpful during the diagnosis. The 3-D images can also be captured and saved for later review.
The latest technology is 4-D ultrasound, which allows the health care provider to visualize the unborn baby moving in real time. With 4-D imaging, a three-dimensional paradigm is continuously updated, providing a "live action" view. These images oft have a golden colour, which helps show shadows and highlights.
Ultrasound images may be captured in nonetheless photographs or on video to document findings.
What are the risks and benefits of ultrasound imaging?
Fetal ultrasound has no known risks other than mild discomfort due to pressure from the transducer on your abdomen or in your vagina. No radiation is used during the procedure.
Transvaginal ultrasound requires covering the ultrasound transducer in a plastic or latex sheath, which may crusade a reaction in women with a latex allergy.
Ultrasound imaging is constantly beingness improved and refined. Equally with whatever test, the results may not be completely authentic. Nonetheless, an ultrasound can provide valuable information to parents and health care providers, helping them manage and care for the pregnancy and the infant. In addition, ultrasound imaging gives parents a unique opportunity to see their infant before nascency, helping them to bond and establish an early relationship.
Fetal ultrasound is sometimes offered in nonmedical settings to provide keepsake images or videos for parents. While the ultrasound procedure itself is considered safe, it is possible that untrained personnel may miss an abnormality or give parents false assurances nearly their infant'southward well-being. It is all-time to have an ultrasound performed by trained medical personnel who can correctly interpret the results. Talk with your doctor or midwife if you have questions.
Amniocentesis
An amniocentesis involves taking a small sample of the amniotic fluid that surrounds the fetus. Information technology is used to diagnose chromosomal disorders and open neural tube defects, such every bit spina bifida. Testing is available for other genetic defects and disorders depending on your family history and the availability of lab testing at the time of the procedure.
Who is an ideal candidate for amniocentesis?
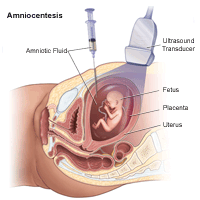
An amniocentesis is generally offered to women between the 15th and 20th week of pregnancy who have an increased risk of chromosomal abnormalities. Candidates include women who volition exist over age 35 at the time of delivery or those who have had an abnormal maternal serum screening examination.
How is an amniocentesis performed?
An amniocentesis involves inserting a long, thin needle through your belly into the amniotic sac to withdraw a small-scale sample of amniotic fluid. The amniotic fluid contains cells shed by the fetus, which comprise genetic data. Although specific details of each procedure may vary, a typical amniocentesis follows this process:
-
Your abdomen volition be cleansed with an antiseptic.
-
Your doctor may or may not give a local anesthetic to numb the skin.
-
Your medico volition use ultrasound applied science to aid guide a hollow needle into the amniotic sac. He or she will withdraw a pocket-sized sample of fluid for lab assay.
You may experience some cramping during or after the amniocentesis. Strenuous activities should be avoided for 24 hours following the procedure.
Women who are pregnant with twins or other higher-society multiples need sampling from each amniotic sac to study each baby. Depending on the position of the babe and placenta, amount of fluid, and woman's anatomy, sometimes the amniocentesis cannot be washed. The fluid is then sent to a genetics lab so that the cells can grow and be analyzed. AFP is likewise measured to rule out an open up neural tube defect. Results are usually available in about 10 days to two weeks, depending on the lab.
Chorionic Villus Sampling (CVS)?
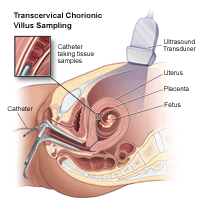
CVS is a prenatal examination that involves taking a sample of some of the placental tissue. This tissue contains the same genetic material every bit the fetus and can be tested for chromosomal abnormalities and some other genetic bug. Testing is available for other genetic defects and disorders, depending on your family history and the availability of lab testing at the fourth dimension of the procedure. Unlike amniocentesis, CVS does non provide information on open up neural tube defects. Therefore, women who undergo CVS too demand a follow-up blood test between 16 and 18 weeks of pregnancy to screen for these defects.
How is CVS performed?
CVS may be offered to women with an increased risk of chromosomal abnormalities or who have a family history of a genetic defect that is testable from the placental tissue. CVS is usually performed betwixt the tenth and 13th week of pregnancy. Although exact methods may vary, the procedure involves the following steps:
-
Your physician will insert a pocket-sized tube (catheter) through your vagina and into your cervix.
-
Using ultrasound technology, your doctor will guide the catheter into place near the placenta.
-
Your doctor will remove some tissue using a syringe on the other end of the catheter.
Your md may also choose to perform a transabdominal CVS, which involves inserting a needle through your abdomen and into your uterus to sample the placental cells. You may feel some cramping during and later on either type of CVS procedure. The tissue samples are sent to a genetic lab for growth and assay. Results are usually bachelor in nigh ten days to 2 weeks, depending on the lab.
What if CVS is not possible?
Women with twins or other higher-society multiples normally need sampling from each placenta. Nonetheless, because of the complication of the procedure and the positioning of the placentas, CVS is not e'er feasible or successful with multiples.
Women who are not candidates for CVS or who did not get accurate results from the procedure may require a follow-up amniocentesis. An active vaginal infection, such as herpes or gonorrhea, will prohibit the procedure. In other cases, the doctor may take a sample that does not have enough tissue to grow in the lab, generating incomplete or inconclusive results.
Fetal Monitoring
During late pregnancy and labor, your medico may want to monitor the fetal heart rate and other functions. Fetal heart rate monitoring is a method of checking the charge per unit and rhythm of the fetal heartbeat. The average fetal middle rate is betwixt 120 and 160 beats per minute. This charge per unit may change every bit the fetus responds to weather condition in the uterus. An abnormal fetal heart charge per unit or pattern may mean that the fetus is not getting enough oxygen or betoken other issues. An abnormal pattern as well may hateful that an emergency cesarean delivery is needed.
How is fetal monitoring performed?
Using a fetoscope (a type of stethoscope) to mind to the fetal heartbeat is the most basic type of fetal heart rate monitoring. Another type of monitoring is performed with a hand-held Doppler device. This is often used during prenatal visits to count the fetal heart charge per unit. During labor, continuous electronic fetal monitoring is often used. Although the specific details of each procedure may vary, standard electronic fetal monitoring follows this process:
-
Gel is applied to your abdomen to act as a medium for the ultrasound transducer.
-
The ultrasound transducer is attached to your abdomen with straps so it can transmit the fetal heartbeat to a recorder. The fetal centre rate is displayed on a screen and printed onto special paper.
-
During contractions, an external tocodynamometer (a monitoring device that is placed over the top of the uterus with a belt) tin can record the pattern of contractions.
When is internal fetal monitoring needed?
On occasion, internal fetal monitoring is needed to provide a more authentic reading of the fetal middle rate. Your purse of waters (amniotic fluid) must be cleaved and your cervix must exist partially dilated to employ internal monitoring. Internal fetal monitoring involves inserting an electrode through the dilated cervix and attaching the electrode to the scalp of the fetus.
Glucose Testing
Glucose testing is used to measure out the level of saccharide in your blood.
A glucose challenge exam is usually conducted between 24 and 28 weeks of pregnancy. Abnormal glucose levels may indicate gestational diabetes.
What is involved in a glucose challenge exam?
The initial one-hr test is a glucose claiming test. If the results are aberrant, a glucose tolerance test is needed.
How is a glucose tolerance exam performed?
You lot may be asked to just drinkable water on the twenty-four hour period the glucose tolerance examination is given. Although the specific details of each procedure may vary, a typical glucose tolerance exam includes the following steps:
-
An initial fasting sample of blood will be drawn from your vein.
-
Yous will be given a special glucose solution to drink.
-
Blood volition exist drawn at various times over the course of several hours to measure the glucose levels in your body.
Group B Strep Culture
Grouping B streptococcus (GBS) is a type of bacteria found in the lower genital tract of about twenty percent of all women. While a GBS infection does non usually cause issues in women before pregnancy, it can crusade serious illness in mothers during pregnancy. GBS may crusade chorioamnionitis (a severe infection of the placental tissues) and postpartum infection. Urinary tract infections caused by GBS can atomic number 82 to preterm labor and birth or pyelonephritis and sepsis.
GBS is the most mutual cause of life-threatening infections in newborns, including pneumonia and meningitis. Newborn babies contract the infection during pregnancy or from the mother's genital tract during labor and commitment.
The Centers for Disease Control and Prevention recommends screening all pregnant women for vaginal and rectal GBS colonization between 35 and 37 weeks gestation. The handling of mothers with certain run a risk factors or positive cultures is of import to reduce the run a risk of transmission of GBS to the babe. Babies whose mothers receive antibiotic treatment for a positive GBS test are 20 times less likely to develop the disease than those without treatment.
Source: https://www.hopkinsmedicine.org/health/wellness-and-prevention/common-tests-during-pregnancy
0 Response to "When Can You Find Out the Sex of the Baby Through Blood Test"
ارسال یک نظر